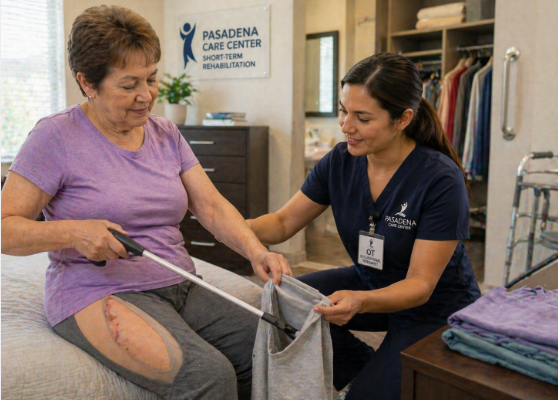
What to Expect During Short-Term Rehab After Hip Replacement
April 28, 2026 0 Comment Category: Short-Term RehabShort-term rehabilitation after hip replacement is a structured, medically supervised recovery program that helps your loved one rebuild strength, relearn movement patterns, and return home safely after surgery. Most people are discharged from the hospital within one to three days of a hip replacement. That is not enough time to recover. The real work happens in the weeks that follow, and where that work takes place matters enormously.
Hip replacement is one of the most common surgical procedures performed in the United States. According to the American Academy of Orthopaedic Surgeons, more than 450,000 total hip replacements are performed each year in the U.S., and that number continues to rise as the population ages. For many families, the surgery itself feels like the hardest part. What comes next is just as important.
Why Short-Term Rehab Follows Hip Surgery
 The hip is a load-bearing joint. After a replacement, the surrounding muscles, tendons, and soft tissue need time to adapt to the new implant. Moving too little slows that process. Moving incorrectly risks dislocation or complications. Short-term rehab exists to thread that needle: guided movement, at the right intensity, with clinical support close at hand.
The hip is a load-bearing joint. After a replacement, the surrounding muscles, tendons, and soft tissue need time to adapt to the new implant. Moving too little slows that process. Moving incorrectly risks dislocation or complications. Short-term rehab exists to thread that needle: guided movement, at the right intensity, with clinical support close at hand.
Going home directly after hospitalization is possible for some people, but it is not the right choice for everyone. If your loved one lives alone, has stairs at home, has limited mobility in their upper body, or has other health conditions that complicate recovery, a short-term rehab stay gives them the supervised environment they need to progress safely before returning to daily life.
What Happens on Day One
The first day in a skilled nursing and rehabilitation setting is focused on two things: safety and baseline assessment. The clinical team reviews surgical records, pain levels, current mobility, and any weight-bearing restrictions ordered by the surgeon. Nothing happens without that foundation.
Physical therapy typically begins within 24 hours of admission. Early movement is not aggressive. The therapist will focus on safe transfers, getting in and out of bed correctly, and controlled walking with a walker or assistive device. The goal is not speed. It is building the muscle memory and confidence to move safely.
The Weekly Arc of Recovery
Short-term rehab after hip replacement follows a general progression. Every person moves through it at a different pace, but the shape of recovery is predictable.
Week one centers on pain management, basic transfers, and short-distance walking. The therapy team watches for signs of complications and adjusts activity based on how your loved one responds. Swelling and fatigue are normal at this stage.
Week two typically brings increased walking distance, stair training if the home environment requires it, and the introduction of exercises that rebuild hip flexor and quadricep strength. Occupational therapy becomes more active during this period, focusing on bathing, dressing, and kitchen tasks.
Week three and beyond is where functional independence gets rebuilt. Longer walks, reduced reliance on assistive devices for some movements, and practice with the specific demands of home life. The team begins discharge planning in earnest, evaluating whether home is ready and whether your loved one is ready for it.
Who Is on the Rehab Team
 Short-term rehab is not one therapist working in isolation. It is a coordinated clinical team working from a shared care plan.
Short-term rehab is not one therapist working in isolation. It is a coordinated clinical team working from a shared care plan.
- Physical therapist leads gait training, strength work, and progressive mobility exercises targeting the hip and surrounding structures.
- An occupational therapist focuses on activities of daily living: how to get dressed safely, how to use adaptive equipment, and how to function independently at home with new limitations.
- Nursing staff monitors wound healing, manages pain, administers medications, and watches for early signs of complications such as infection, blood clots, or implant stress.
- The attending physician or medical director oversees the overall plan, coordinates with the surgeon, and manages any medical issues that arise during the stay.
- Social worker or discharge planner coordinates the transition home, arranges follow-up care, and connects families with any equipment or in-home support they will need after discharge.
Hip Precautions and Why They Matter
Most hip replacement surgeries come with a set of movement restrictions called hip precautions. These are not optional guidelines. Violating them in the early weeks can cause the new joint to dislocate, which requires emergency intervention and can set recovery back significantly.
Common posterior approach precautions include avoiding bending the hip past 90 degrees, not crossing the legs, and not rotating the foot inward. The rehab team teaches these precautions on day one and reinforces them throughout every therapy session and every daily activity. When your loved one goes home, they need to carry these rules with them. The rehab team will make sure they do.
Understanding the difference between short-term rehabilitation and other post-acute options helps families make the right choice. The table below compares the primary settings available after hip replacement surgery.
| Setting | Level of Medical Support | Therapy Frequency | Best For |
|---|---|---|---|
| Skilled nursing and rehab facility | 24-hour nursing, physician oversight | Daily PT and OT, 5-7 days per week | Complex recovery, limited home support, multiple health conditions |
| Inpatient rehabilitation hospital | Intensive medical supervision | 3+ hours of therapy per day | Patients who can tolerate high-intensity therapy immediately post-surgery |
| Home health care | Periodic nurse or therapist visits | 2-3 visits per week | Strong home support system, limited complications, high baseline mobility |
| Outpatient therapy | None between sessions | 2-3 sessions per week | Later-stage recovery, independent living, reliable transportation |
Does Medicare Cover Short-Term Rehab After Hip Replacement
For most people, yes. Medicare Part A covers short-term skilled nursing facility care following a qualifying hospital stay of at least three inpatient days. Hip replacement almost always meets that threshold. Under Medicare Part A, days one through twenty are covered at no cost to the resident. Days twenty-one through one hundred require a daily copayment, which in 2024 is $194.50 per day. After day one hundred, Medicare coverage ends.
Medi-Cal coverage for short-term rehab varies based on the individual’s eligibility and the facility’s certification. Families should confirm coverage with the admissions team before placement. A good facility will walk you through the benefits before your loved one ever arrives.
For a full breakdown of how Medicare covers skilled nursing care and what the qualification requirements look like, the Centers for Medicare and Medicaid Services publishes detailed guidance at medicare.gov.
What Good Progress Actually Looks Like
 Families sometimes expect a straight line upward. Recovery rarely works that way. A day of fatigue or increased pain does not mean something is wrong. It often means the body is doing the hard work of adaptation. The rehab team tracks progress across a range of clinical measures, not just how far someone walked on a given day.
Families sometimes expect a straight line upward. Recovery rarely works that way. A day of fatigue or increased pain does not mean something is wrong. It often means the body is doing the hard work of adaptation. The rehab team tracks progress across a range of clinical measures, not just how far someone walked on a given day.
Real milestones to watch for: independent transfers without verbal cueing, walking 150 feet with a walker without stopping, ascending and descending a full flight of stairs with supervision, and completing a simulated home task without assistance. When those milestones are consistently met, discharge is close.
If you want to understand what the full short-term rehabilitation process looks like from admission through discharge, the short-term rehabilitation services page covers the clinical framework in detail.
Questions Families Ask Before the Stay Begins
How long does short-term rehab after hip replacement usually last?
Most people complete short-term rehab in two to four weeks. The exact length depends on how quickly strength and mobility return, whether complications arise, what the home environment looks like, and the level of support available after discharge. Some residents progress faster; others need additional time. The team reassesses the care plan regularly and adjusts the projected discharge date based on clinical progress, not a predetermined schedule.
Can my loved one go straight home from the hospital instead of to a rehab facility?
Some people do, particularly those who are younger, have strong physical baselines before surgery, and have capable caregivers at home. For many older adults, however, going home too soon increases the risk of falls, complications, and readmission. A rehabilitation facility provides round-the-clock clinical monitoring, daily therapy, and a supervised environment during the most vulnerable window of recovery. The surgeon and hospital discharge team will make a recommendation, but families should also evaluate what home truly looks like in those first two weeks.
What should my loved one bring to a short-term rehab stay?
Comfortable, loose-fitting clothing that is easy to put on and take off is essential. Slip-resistant footwear with good support. Any personal items that make the space feel familiar. All current medications in their original bottles, or a complete medication list. Insurance cards and a photo ID. The admissions coordinator will provide a full packing checklist, but the most important thing is that your loved one arrives with what they need to feel safe and comfortable.
Will the therapists coordinate with my loved one’s surgeon?
Yes. The rehabilitation team works from the surgeon’s post-operative orders, which specify weight-bearing status, hip precautions, and any restrictions. If questions arise during the stay, the medical director or attending physician communicates directly with the surgeon. Families should bring any written discharge instructions from the hospital to the admissions appointment so the team has a complete picture from day one.
What happens when short-term rehab ends?
Discharge planning begins early in the stay, not in the final days. The team evaluates the home environment, coordinates any equipment needs such as a raised toilet seat or shower chair, arranges follow-up outpatient therapy if needed, and provides detailed instructions for continuing exercises at home. Some residents transition to a longer-term assisted living arrangement if returning home is not yet safe. The goal is a planned, supported discharge, not an abrupt one.
How many therapy sessions will my loved one receive each day?
In a Medicare-certified skilled nursing facility, residents typically receive one to two therapy sessions per day, five to seven days per week. Sessions generally run 30 to 60 minutes each. The exact schedule is based on the individual care plan and the resident’s tolerance on any given day. Fatigue is real in early recovery, and the therapy team calibrates the schedule accordingly. Rest is part of the treatment plan.
Choosing the Right Place for Recovery
The facility where your loved one recovers shapes everything about how that recovery goes. Ask about therapy staffing ratios, how often the attending physician is on site, what the process is for communicating with families, and how discharge planning is handled. The answers tell you a great deal about how a facility operates.
Foothill Heights Care Center in Pasadena has been providing short-term rehabilitation and skilled nursing care to families across the San Gabriel Valley for decades. If your loved one is preparing for hip replacement surgery and you want to understand what recovery at Foothill Heights looks like, call (626) 798-1111 to speak with our admissions team or to schedule a tour before the surgery date arrives.
Foothill Heights Care Center
1515 North Fair Oaks Ave
Pasadena, CA 91103
(626) 798-1111
Serving Pasadena, Arcadia, Monrovia, Temple City, San Marino, Alhambra, Sierra Madre, and Altadena

leave A comment